Have a Question?
The Gut-Brain Connection: Can Diet Influence Parkinson’s Disease Symptoms?

April marks a significant period for Parkinson’s disease awareness, highlighted by World Parkinson’s Day on 11 April and a month-long focus on education and advocacy. As one of the fastest-growing neurological conditions globally, Parkinson’s continues to place increasing pressure on individuals, families, and healthcare systems.
While traditionally associated with motor symptoms, Parkinson’s is now understood to be more complex. Emerging research is drawing attention to the gut-brain connection, suggesting the digestive system could play a role in how the condition develops and progresses. This has led to increasing interest in how diet and gut health may help manage symptoms and improve quality of life.
Understanding Parkinson’s Disease
Parkinson’s disease is a progressive neurological condition that affects movement and coordination. It occurs when dopamine-producing brain cells gradually degenerate, reducing the brain’s ability to control smooth and balanced movement.
An estimated 219,000 Australians are living with Parkinson’s or a related condition. Each day, between 38 and 50 Australians are diagnosed, more than one person every hour, resulting in over 19,500 new cases each year.
Although commonly associated with older age, around 10–20% of cases occur in younger individuals aged between their 20s and 50s.
More than 1,100 Australians under 65 receive a diagnosis annually. The condition affects slightly more men (52%) than women (48%), and with incidence rates rising by approximately 4% each year.
Common Symptoms
Parkinson’s presents with both motor and non-motor symptoms:
- Motor symptoms may include tremors, muscle stiffness, and slowed movement.
- Non-motor symptoms can also occur, such as constipation, mood changes, and sleep disturbances, which may impact overall quality of life.
What is the Gut-Brain Connection?
The gut-brain connection, also known as the gut-brain axis, refers to the bidirectional communication between the gastrointestinal system and the central nervous system. This interaction is facilitated through several pathways, including:
- The vagus nerve, which directly connects the gut to the brain
- The immune system, which responds to inflammation and infection
- Hormonal signalling, influencing mood and bodily functions
- The gut microbiome, consisting of trillions of microorganisms that play a role in digestion, immunity, and neurological processes
This system allows the gut and brain to influence each other continuously. In the context of Parkinson’s, this connection is particularly relevant because gastrointestinal symptoms often precede motor symptoms by years.
The Link Between Gut Health and Parkinson’s
Early Gut Changes in Parkinson’s
Digestive issues, particularly constipation, are often among the earliest signs of Parkinson’s. Emerging research suggests that changes associated with Parkinson’s may begin in the gut, sometimes years before motor symptoms appear.
Alpha-Synuclein and the Gut
Parkinson’s is linked to the buildup of a protein called alpha-synuclein. This protein can form abnormal clumps that disrupt normal cell function. Some research indicates that these changes may originate in the gut and travel to the brain via the vagus nerve.
Gut Microbiome Imbalance
People with Parkinson’s often show differences in their gut bacteria composition. This imbalance may contribute to increased inflammation and can influence the severity of both digestive and neurological symptoms.
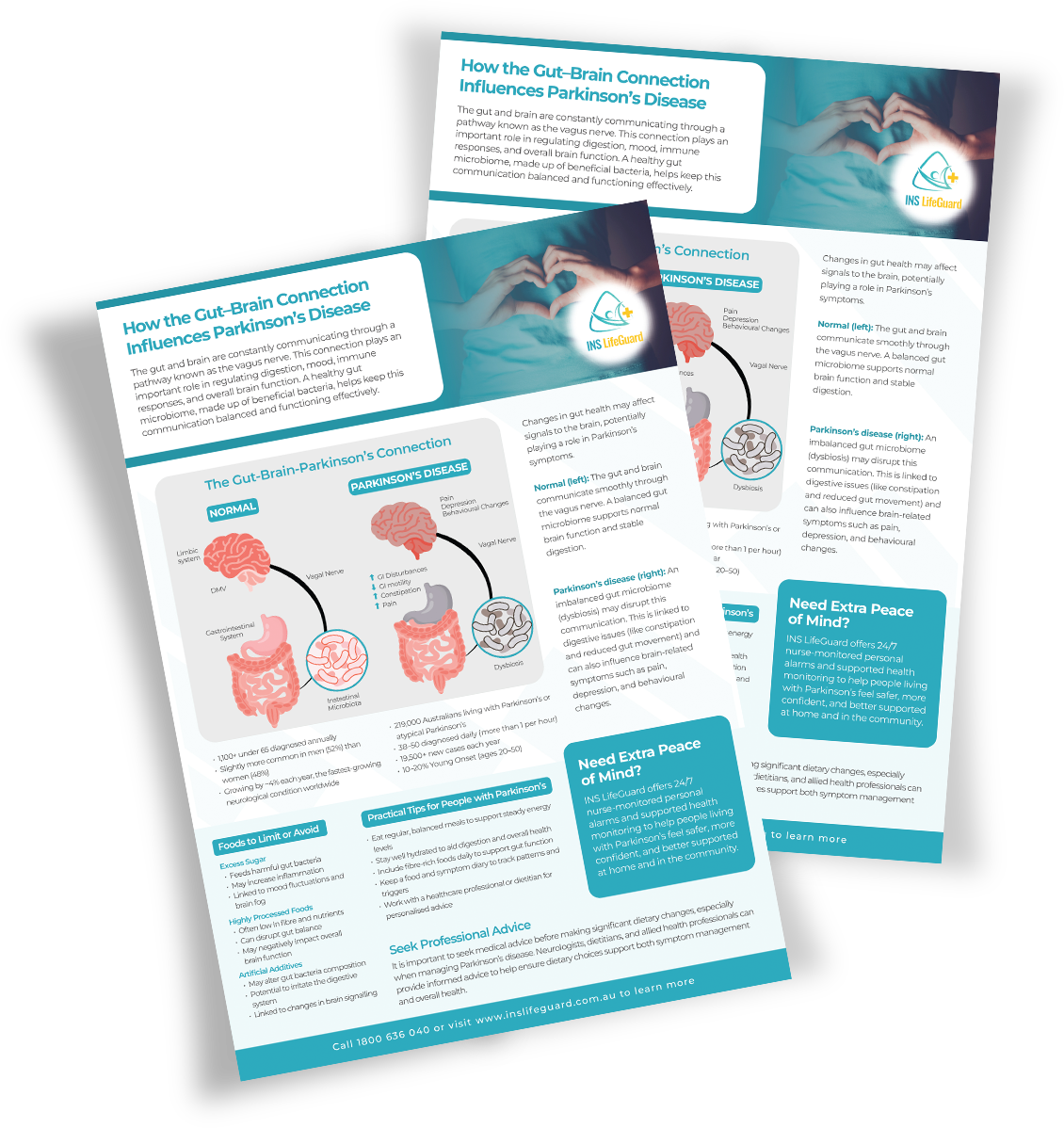
How the Gut–Brain Connection Influences Parkinson’s Disease
Gaining a deeper understanding of how gut health may influence Parkinson’s disease can help individuals better manage symptoms and support overall well-being. Our free downloadable resource provides a clear overview of the gut–brain–Parkinson’s connection, including early gut-related changes, and dietary considerations.
Designed for easy reading, this resource offers practical insights for those living with Parkinson’s, as well as their families and carers.
The Role of Nutrition in Brain Health
Nutrition plays an important role in supporting brain function and overall neurological health. A well-balanced diet provides essential nutrients that help maintain brain activity, support energy levels, and contribute to general well-being.
Anti-Inflammatory Eating
An anti-inflammatory diet may help reduce inflammation in the body, which is linked to many chronic conditions. Foods such as fruits, vegetables, whole grains, and healthy fats like olive oil and fish can support both gut and brain health.
The Mediterranean Diet and Parkinson’s
The Mediterranean diet has been widely studied for its potential benefits in brain health. Research suggests it may help improve symptoms or slow progression in Parkinson’s. This approach focuses on whole foods, including fresh produce, lean proteins, healthy fats, and minimal processed foods.
Fibre and Gut Health
Fibre plays a key role in maintaining healthy digestion and supporting a balanced gut microbiome. For people living with Parkinson’s, adequate fibre intake may help manage constipation and improve overall digestive comfort.
Probiotics and Fermented Foods
Probiotics and fermented foods may support the growth of beneficial gut bacteria. Foods such as yoghurt, kefir, and kimchi can help maintain gut balance, which may influence both digestive and neurological health.
Protein and Medication Interactions
Protein can affect how Parkinson’s medications, particularly levodopa, are absorbed in the body. Managing the timing of protein intake in relation to medication may help improve its effectiveness and symptom control.
Practical Dietary Tips for People with Parkinson’s
Maintaining supportive daily habits can help improve overall well-being and symptom management:
- Eat regular, balanced meals to support consistent energy levels
- Stay well hydrated to assist digestion and reduce constipation
- Include fibre-rich foods daily to promote gut health
- Keep a food and symptom diary to identify patterns and triggers
- Work with a healthcare professional or dietitian for personalised support
It is important to seek medical advice before making significant dietary changes, particularly when managing a condition like Parkinson’s. Healthcare professionals can help ensure that dietary choices support both symptom management and overall health.
Supporting Safety, Confidence and Independence
Living with Parkinson’s disease can be challenging, not only for those diagnosed but also for the families and loved ones who support them. As symptoms change over time, having the right support in place can make a meaningful difference to safety, confidence and independence.
For some people, added reassurance may come from having a monitored personal alarm. As Australia’s only nurse-monitored personal alarm provider, INS LifeGuard offers in-home and mobile personal alarm options that provide access to qualified nurses at the press of a button, with automatic fall detection and telehealth services available on selected devices. For people living with reduced mobility, balance changes, or uncertainty when alone, this can offer extra peace of mind at home and in the community.
Conclusion
Although diet is not a cure, it can play a meaningful role in everyday life by supporting strength, digestion, mobility, and overall well-being. Small, informed changes may make a real difference, helping people feel more confident and supported in their daily routines.
Through greater awareness, continued education and the right support, individuals and families navigating Parkinson’s disease can take positive steps to protect quality of life at every stage.

About
INS LifeGuard is the only 24/7 nurse on-call personal and medical monitoring in Australia. We provide monitoring technology for both in the home and on the go and can also monitor other provider's equipment. Our services are suitable for anyone wanting support to stay independent such as the elderly, those with medical conditions and disabilities plus enhancing safety and security for lone workers.

















